Program Overview:
Angiographic Work (for the detection of arterial disease and malformations)
- Angio Brains
- Angio Neck
- Angio Chest (with Cardiac Gating Procedure if applicable)
- Angio Abdomen
- Angio Pelvis
- Angio Extremeties (both upper and lower)
Breast Division and Services
Diagnostic Imaging / Xray:
- General Radiography
- Trauma Radiography
- OR Radiography
- Mobile Radiography
- Fluoroscopy Procedures (includes Barium Enemas, GI studies, Modified Barium Studies with Speech Language Pathologist)
- Special Procedures (includes : Arthrography, , Voiding Cystograms, Joint Injections (for pain management), Hysterosalpingograms)
- Bone Densitometry
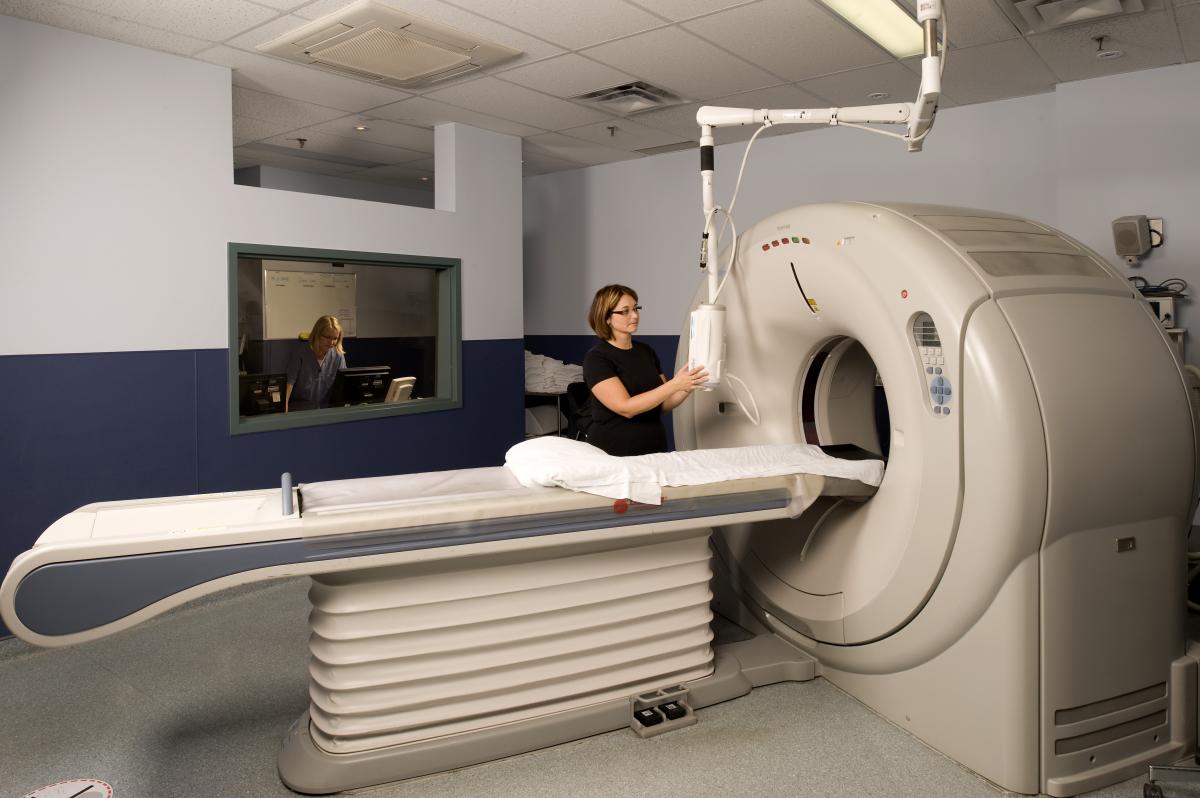 General CT Scanning:
General CT Scanning:
- Head ( CT perfusion Studies included)
- Cervical spine
- Thoracic Spine
- Lumbar Spine
- Abdomen and Pelvis Scanning
Specialized Scanning of the Following:
- Renal Stones
- CT Colonoscopy
- CT Fluoro for Special Procedures (Biopsies of the Lungs, Abdomen, Pelvis, Abcess Drainages and other Special Procedures)
Orthopedic Scanning:
All extremeties for the purpose of Surgical Planning and Malformations.
MRI
Magnetic Resonance Imaging (MRI) is a painless, non-invasive diagnostic imaging technology that uses a strong magnetic field to produce images. MRI scans can provide information about the brain, spine, joints, organs and vessels.
MRI can also help differentiate between different tissues in the body that are not visible with any other imaging modality. Some MRI examinations may require an injection of contrast to help visualize structures more clearly. The contrast media is called Gadolinium, and is very safe and the risks will be discussed with you by the technologist. If you are required to have an exam with contrast, you will be asked to go for blood work prior to the exam, to check for renal function. Most MRI exams will take between 20- 45 minutes; however there are some that can take up to an hour. If there is more than one body part being examined, the scan can be longer than 1 hour. Please inquire at booking time. The preparation for an MRI is that you have nothing to eat or drink 4 hours prior to your exam. Medications can be taken with a small amount of water.
The MRI technologist will explain the procedure to you and confirm the information provided on the screening form. Once the procedure has been explained you will be instructed to change into a hospital gown. Lockers are available to lock up your belongings and valuables. When it is time for the exam, the technologist will escort you into the MRI room, where you will lie down on the table. Headphones or earplugs will be given to you to protect your ears from the noise that the machine makes. You will also be given an emergency bell so that if at anytime you need to come out of the scanner, all you have to do is squeeze the bell and the technologists will come and take you out.
It is very important that you stay very still while having your scan done, so that the images are clear. If you move the images will be blurry. Please be aware that there is a table weight restriction of 400 lbs with a maximum width of 60 cm. For optimal images it is necessary for the body part being imaging to be in the middle of the MRI scanner. For patient specific questions please contact the MRI Booking Department.
MRI Services provided:
- Breast MRI (which will include Breast Biopsy in the near future)
- Abdominal/Pelvic MRI
- Head and Neck MRI
- Musculoskeletal MRI
- Neuro and Neurovascular MRI
MyPocketHealth
As of May 29 2018 the Timmins and District Hospital, and its NORrad Partner sites, will be offering an online platform for patients to access their Diagnostic Imaging studies and reports through a partnership with PocketHealth
Once enrolled, patients will have full control to view and share their imaging records.
How does it work?
-
Patients have the option to enroll themselves ONLINE at www.mypockethealth.com/NORrad or by submitting a Paper Enrollment form to the PACS Film Library Clerk.
-
Once enrolled, the patient receives an access email with a secure link to their entire NORrad Imaging history.
From their PocketHealth account patients can:
-
View their Imaging Records (imaging + reports).
-
Download their original DICOM imaging.
-
Share their imaging records with any healthcare professional’s email address.
-
Burn a CD/USB with a diagnostic viewer for their physician.
-
Electronically request records from other imaging clinics and hospitals across Ontario.
Technical Issues:
Patient’s experiencing technical Issues should contact PocketHealth Support:
- Email: help@mypockethealth.com
- Phone: 1-855-381-8522
What does the patient side of the platform look like?
- A video walkthrough of the patient-facing part of the platform: https://youtu.be/aJoEarR3x_A
Will we still be able to burn CD?
- Yes. CD burning will still be an option for patients. PocketHealth is an alternative solution.
How are patient records protected?
With respect to privacy, the PocketHealth sign up (electronic and paper copy) requires that the patient absolve the participating Hospitals of any liability with respect to the data release. This is no different than us handing over a CD to the patient with all of their imaging data. Once in their possession, it is their responsibility to keep it secure. PocketHealth is simply a way for patients to access their imaging data (like a CD) in a “cloud”.
Nuclear Medicine
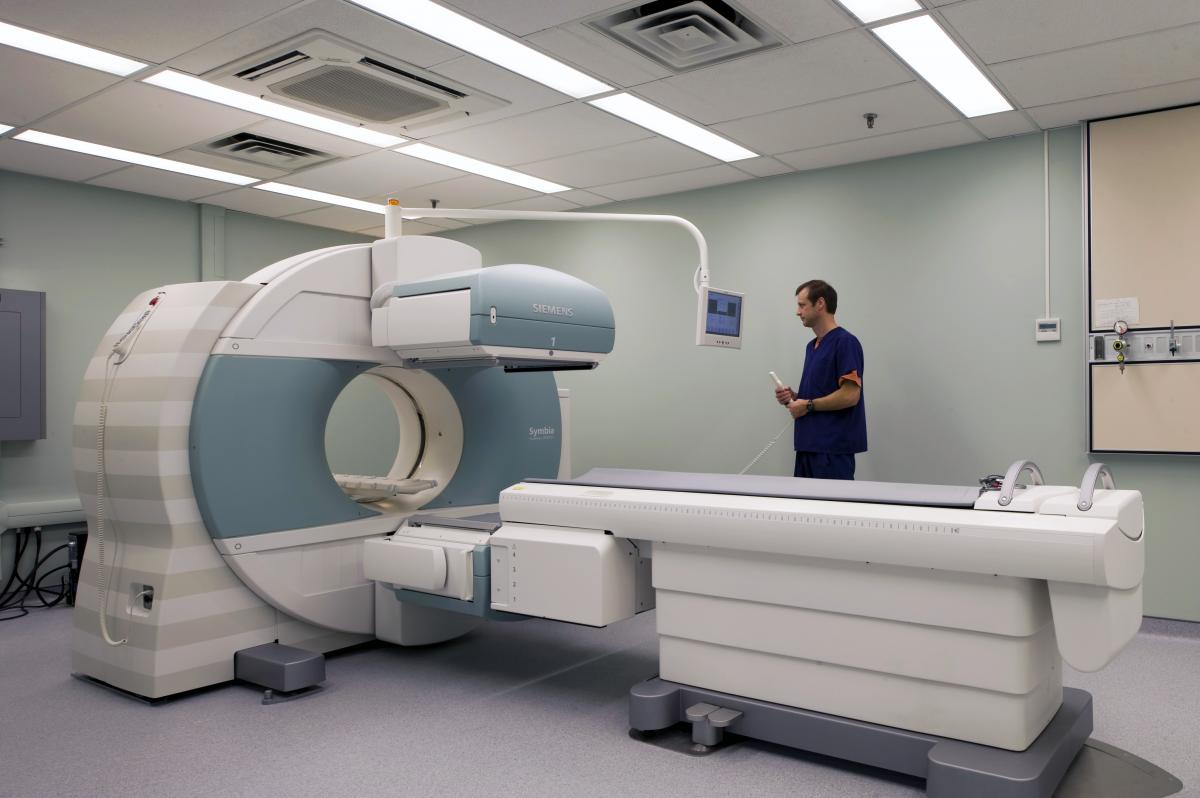 Nuclear medicine scans use small amounts of radioactive dye (tracer) to highlight areas of concern, such as cancer cells or infection. Pictures can than be taken of these areas.
Nuclear medicine scans use small amounts of radioactive dye (tracer) to highlight areas of concern, such as cancer cells or infection. Pictures can than be taken of these areas.
There are many types of nuclear medicine scans, including:
- Bone Scan
- Cardiac Imaging
- Gallium Scan
- Gallbladder Scan
A special dye called a radioactive isotope, or tracer, is given through an IV. This tracer contains a small amount of radiation, about the same amount as an x-ray. The dye travels through the body and gathers in the area of the body being examined. When the dye has gathered in a tumor or organ, it gives off energy in the form of gamma rays. A special scanner or camera then captures images based on the gamma rays. Nuclear medicine scan pictures can detail both the function and structure of tissues and organs in the body.
The small amount of radioactive material will decay over time. It may also pass out of your child’s body through urine or stool during the first few hours or days following the test. Drinking plenty of water may help flush the radioactive material out of the body. Follow the instructions given to you by the nuclear medicine staff.
Nuclear medicine scans do not hurt. Allergic reactions to the tracers can occur, but they are extremely rare and are usually mild.
Bone scan
A bone scan is a nuclear scanning test to find certain abnormalities in bone. It is primarily used to help diagnose a number of conditions relating to bones, including: cancer of the bone or cancers that have spread (metastasized) to the bone, locating some sources of bone inflammation (e.g. bone pain such as lower back pain due to a fracture), the diagnosis of fractures that may not be visible in traditional X-ray images, and the detection of damage to bones due to certain infections and other problems.
Cardiac Imaging
Myocardial perfusion scan (also referred to as MPI) is a nuclear medicine procedure that illustrates the function of the heart muscle (myocardium).[1]
It evaluates many heart conditions from coronary artery disease (CAD) to hypertrophic cardiomyopathy and myocardial wall motion abnormalities. The function of the myocardium is also evaluated by calculating the left ventricular ejection fraction (LVEF) of the heart. This scan is done in conjunction with a cardiac stress test.
Planar techniques, such as conventional scintigraphy, are rarely used, SPECT/CT is more commonly performed. With multihead SPECT/CT systems, imaging can often be completed in less than 10 minutes. With SPECT/CT, interior and posterior abnormalities and small areas of infarction can be identified, as well as the occluded blood vessels and the mass of infarcted and viable myocardium.
A MUGA scan (Multi Gated Acquisition Scan) is a time-proven nuclear medicine test designed to evaluate the function of the right and left ventricles of the heart, thus allowing informed diagnostic intervention in heart failure. This modality uniquely provides a cine image of the beating heart, and allows the interpreter to determine the efficiency of the individual heart valves and chambers, left ventricular ejection fraction. MUGA/Cine scanning represents a robust adjunct to the now more common echocardiogram.
Kidney Scan
A renal (kidney) scan is a diagnostic procedure that uses nuclear medicine to examine the anatomy and functioning of your kidneys. A renal scan is also called a renal scintigraphy, renal imaging, or a renogram.
During this procedure, a radioactive material, called a radioisotope or radionuclide “tracer,” is injected into your vein. The radioisotope releases gamma rays, which a gamma camera or scanner can detect from outside the body.
The gamma camera scans the kidney area. It tracks the radioisotope and measures how it is processed by the kidneys. The camera also works together with a computer to create images. These images detail the structure and functioning of the kidneys, based on how they interact with the tracer.
Images from a renal scan can show structural and functional abnormalities, helping doctors to diagnose a kidney problem in its earlier stages—without invasive techniques or surgery.
Lung Scan
A ventilation/perfusion lung scan, also called a V/Q lung scan, is a type of medical imaging using scintigraphy and medical isotopes to evaluate the circulation of air and blood within a patient's lungs, in order to determine the ventilation/perfusion ratio. The ventilation part of the test looks at the ability of air to reach all parts of the lungs, while the perfusion part evaluates how well blood circulates within the lungs.
This test is most commonly done in order to check for the presence of a blood clot or abnormal blood flow inside the lungs (such as a pulmonary embolism or PE), although computed tomography with radiocontrast is now more commonly used for this purpose. The V/Q scan may be used in some circumstances where radiocontrast would be inappropriate, as in renal failure
Thyroid Scan
A thyroid scan uses a radioactive tracer and a special camera to measure how much tracer the thyroid gland absorbs from the blood. The tracer can be swallowed or can be injected into a vein. It travels through your body, giving off radiation signals. The camera "sees" the signals and can measure how much tracer the thyroid absorbs from the blood.
A thyroid scan can show the size, shape, and location of the thyroid gland. It can also find areas of the thyroid gland that are overactive or underactive. The camera takes pictures of the thyroid gland from three different angles. The radioactive tracer used in this test is either iodine or technetium.
A radioactive iodine uptake (RAIU) test may also be done to find problems with how the thyroid gland works, such as hyperthyroidism. Another type of thyroid scan, a whole-body thyroid scan, may be done for people who have had thyroid cancer that has been treated. The whole-body scan can check to see if cancer has spread to other areas of the body.
Gallbladder Scan
A gallbladder scan, also known as: Hepatobiliary Iminodiacetic Acid HIDA, Paraisopropyl Iminodiacetic Acid PIPIDA, or Diisopropyl Iminodiacetic Acid DISIDA scan is a nuclear imaging procedure to evaluate the health and function of the gallbladder. A radioactive tracer, usually a 99
Tc-iminodiacetic acid chelate complex, is injected through any accessible vein, then allowed to circulate to the liver, where it is excreted into the biliary system and stored by the gallbladder and biliary system.
In the absence of disease, the gallbladder is visualized within 1 hour of the injection of the radioactive tracer. If the gallbladder is not visualized within 4 hours after the injection, this indicates either cholecystitis or cystic duct obstruction. This investigation is usually conducted after an ultrasound examination of the abdominal right upper quadrant for pain. If the non-invasive ultrasound examination fails to demonstrate gall stones (or other obstruction to the gall bladder or biliary tree) in an attempt to establish a cause of right upper quadrant pain, this cholescintigraphy scan can be performed as a more sensitive and specific test. Cholescintigraphy scans are not generally done first line due to their increased cost and invasiveness.
Cholescintigraphy for acute cholecystitis has sensitivity of 97%, specificity of 94%. Several investigators have found the sensitivity being consistently higher than 90% though specificity has varied from 73%- 99%, yet compared to ultrasonography, cholescintigraphy has proven to be superior. The scan is also important to differentiate between Neonatal Hepatitis and Biliary atresia, because an early surgical intervention in form of Kasai portoenterostomy or Hepatoportoenterostomy can save the life of the baby as the chance of a successful operation after 3 months seriously decreases.
Radiology Students/Clinical Instructors:
Radiology students are here for one year clinical placement from January to December. We accept 2-3 Cambrian College students and 2 College Boreal Students annually.
We have 2 clinical instructors available: Vanessa Backer and Line Cloutier. Vanessa is the Education Team Leader for the department. The instructors collaborate with the program coordinator's and follow their program curriculum.
Students are evaluated clinically and didactically by the instructors. Evaluation tools are set in place by the colleges. Students are evaluated on their performance and given ongoing feedback from their instructors on a weekly basis. The instructors set time aside to review material in a classroom setting.
Ultrasound
TADH currently has six(seven) ultrasound units located on site. The department is proud to have the latest in technology with our Toshiba units. We have 2 Aplio XG units and 4 Toshiba Aplio 500 units.
We perform a variety of examinations including but not limited to: abdominal, obstetrical, gynecological, testicular, trans rectal ultrasound of the prostate, breast, thyroid, venous Doppler studies, salivary glands, pediatric sonography and special procedures(guided ultrasound biopsies)
Unlike x-ray exams which use ionizing radiation to create images, ultrasound is a safe test performed by sonographers using sound waves to produce an images of organs for diagnostic purposes. The ultrasound department also provides interventional services in the form of biopsies. These images are reviewed by radiologists who provide each patient/referring physician with a verified report of the findings.
We are very fortunate to have an accredited vascular laboratory. We are currently seeking accreditation for our echocardiography laboratory.
Our staff is registered in the following areas:
- Abdomen & Small Parts
- Obstetrics & Gynecology
- Neurosonography
- Vascular
- Adult echocardiography
- Breast sonography
We are also seeking registry in the specialty of musculo-skeletal ultrasound.
Service in our ultrasound department is staffed weekly from 7:00 am to 8:30pm with emergency on-call coverage after hours.
As a training facility, we currently accept two ultrasound students for completion of their clinical rotation, students from Cambrian College and College Boreal in Sudbury. This helps our northern communities with finding qualified sonographers and with staff retention.
Continuing education is very important in our modality and we are all current with the Canadian Association of Registered Diagnostic Ultrasound Professionals(C.AR.D.U.P.) and the American Registry of Diagnostic Medical Sonographers (A.R.D.M.S)